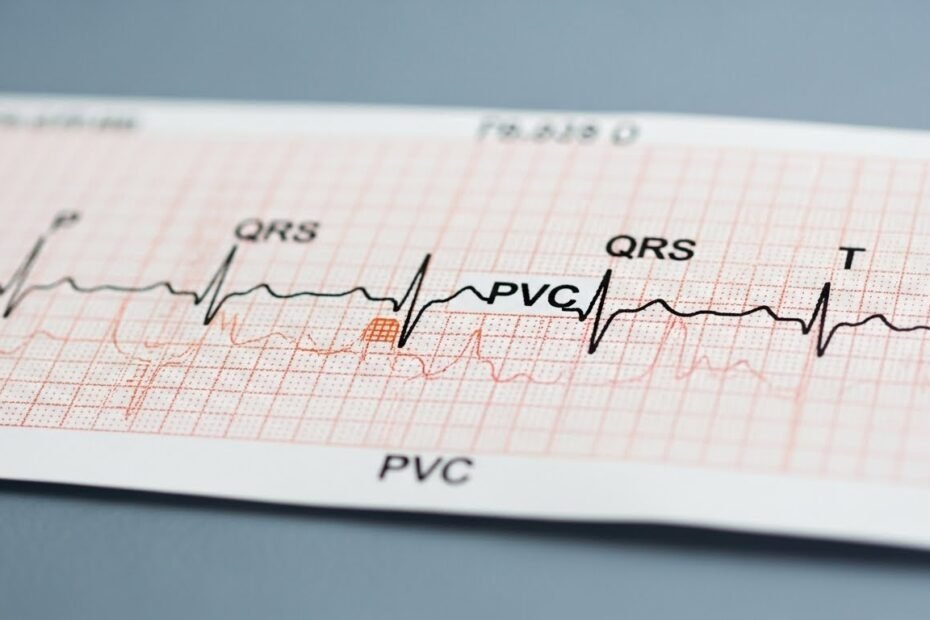
Introduction to PVC on EKG Strip
If you’ve ever looked at an EKG strip, you may have noticed various waveforms and patterns that tell a story about the heart’s activity. One of the most significant anomalies that can appear is the Premature Ventricular Complex (PVC). Understanding PVC on an EKG strip is crucial for both healthcare professionals and patients. It offers insights into heart health and potential underlying issues.
PVCs are not uncommon; in fact, many people experience them at some point in their lives. They can be benign or indicative of more serious problems. Therefore, recognizing their appearance on an EKG strip can help in making informed decisions regarding cardiovascular health. In this article, we’ll dive deep into what PVCs are, how they manifest on an EKG strip, their causes, symptoms, and treatment options.
What is a PVC?
A Premature Ventricular Complex is an early heartbeat originating in the ventricles. This means that they disrupt the normal rhythm of the heart. Imagine your heart as a well-coordinated orchestra. When a PVC occurs, it’s like a musician playing out of sync, causing a temporary disarray. PVCs can happen randomly or in patterns, and while they may feel alarming, many people live with them without any serious issues.
What causes these disruptions? PVCs can arise from various factors including stress, caffeine intake, certain medications, or underlying heart conditions. Sometimes, they occur in healthy individuals without any identifiable cause. Understanding the context in which PVCs appear is essential for healthcare providers when interpreting EKG results.
How PVCs Occur
PVCs occur when the ventricles contract prematurely, ahead of the normal heartbeat. This results in an irregular heartbeat followed by a compensatory pause. This pause allows the heart to reset its rhythm, which can sometimes create a sensation of a ‘skipped beat’ in patients. The EKG strip will show a wide and bizarre QRS complex, often without a preceding P wave, which is characteristic of PVCs.
Identifying PVCs on an EKG Strip
Identifying PVCs on an EKG strip requires a trained eye. The characteristic signs include a wide QRS complex that appears earlier than expected, which disrupts the regular rhythm. The QRS complex typically lasts longer than 0.12 seconds and is often followed by a compensatory pause. This can be likened to a hiccup in an otherwise smooth conversation.
When interpreting an EKG strip, healthcare professionals look for patterns. PVCs can appear as isolated events or in patterns such as bigeminy (every other beat is a PVC) or trigeminy (every third beat is a PVC). These patterns can help determine the significance of the PVCs and guide further investigation or treatment.
How to Read an EKG Strip for PVCs
Reading an EKG strip for PVCs involves the following steps:
- Step 1: Locate the QRS complexes on the strip.
- Step 2: Identify any wide QRS complexes that appear prematurely.
- Step 3: Check for the absence of P waves preceding the PVCs.
- Step 4: Measure the duration of the QRS complex; if it’s over 0.12 seconds, it’s likely a PVC.
- Step 5: Look for patterns such as bigeminy or trigeminy.
This systematic approach helps ensure accurate identification of PVCs and assists in developing an effective treatment plan if necessary.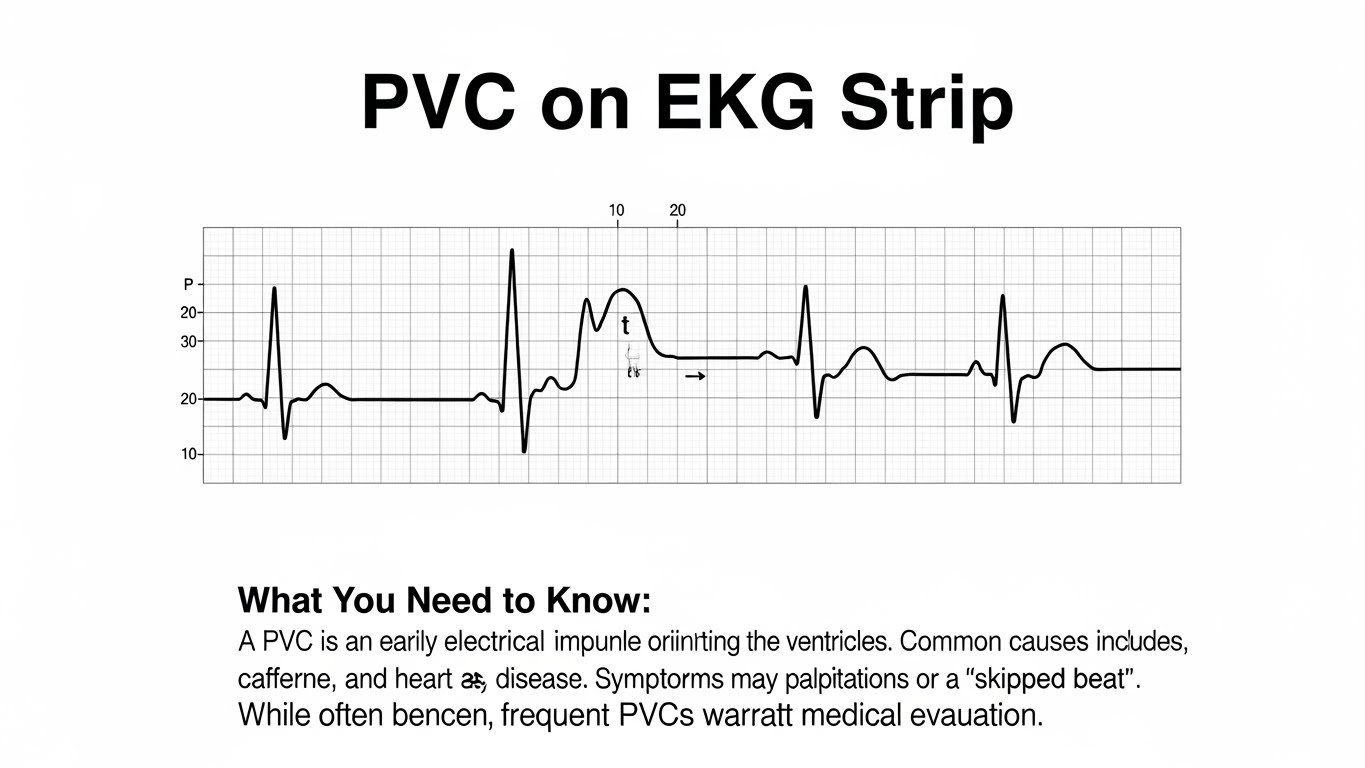
Causes of PVCs
The causes of PVCs can be diverse, ranging from benign to more serious conditions. In many cases, PVCs occur due to lifestyle factors or emotional stress. Common triggers include excessive caffeine consumption, smoking, alcohol intake, and high levels of stress or anxiety.
However, PVCs can also be associated with underlying heart conditions. For example, structural heart diseases, electrolyte imbalances, or ischemic heart disease may lead to frequent PVCs. Understanding these causes is essential for patients and healthcare providers alike, as it guides the decision-making process for treatment and lifestyle modifications. Understanding EKG Strips: A Comprehensive Guide
Risk Factors for PVCs
Several risk factors may increase the likelihood of experiencing PVCs:
- Age: Older adults may have an increased prevalence of PVCs.
- Heart Disease: Patients with a history of heart disease are at a higher risk.
- High Blood Pressure: Hypertension can lead to structural changes in the heart.
- Electrolyte Imbalances: Low levels of potassium or magnesium can trigger PVCs.
- Caffeine and Stimulants: Substances that stimulate the heart can provoke PVCs.
Recognizing these risk factors can aid in prevention and management strategies.
Symptoms Associated with PVCs
Many individuals with PVCs may not experience noticeable symptoms. However, some people report sensations like palpitations, a fluttering feeling in the chest, or a sense of skipped beats. These symptoms can be unsettling, leading to increased anxiety, which can ironically exacerbate the situation.
In more severe cases, frequent PVCs may lead to complications such as reduced cardiac output or even heart failure. Therefore, it’s essential for anyone experiencing significant symptoms to seek medical advice. The relationship between symptoms and the frequency or patterns of PVCs can help healthcare providers assess the need for further evaluation.
When to Seek Medical Attention
While occasional PVCs are generally harmless, certain situations warrant immediate medical attention:
- If you experience chest pain or discomfort alongside PVCs.
- If you feel lightheaded or faint during episodes.
- If PVCs increase in frequency or change in pattern.
- If you have a history of heart disease and begin experiencing new symptoms.
Recognizing these warning signs can be crucial for timely intervention.
Diagnosis of PVCs
Diagnosing PVCs typically starts with a thorough patient history and physical examination. Healthcare providers may take a detailed account of symptoms and any potential triggers the patient has noticed. Following this, an EKG is performed to visualize the heart’s electrical activity. This is where the PVC on the EKG strip becomes evident.
In some cases, healthcare providers may recommend further testing, such as a Holter monitor, which records heart activity over 24 hours or longer. This can capture intermittent PVCs that may not show up during a standard EKG. These diagnostic methods help create a comprehensive picture of the patient’s heart health.
Advanced Diagnostic Tools
Beyond the standard EKG, advanced tools may be employed for diagnosis:
- **Echocardiogram:** This imaging test assesses heart structure and function.
- **Stress Test:** Evaluates how the heart responds to physical exertion.
- **Electrophysiological Study:** Involves inserting catheters into the heart to study electrical signals.
These tests can provide deeper insights into the heart’s condition and the significance of PVCs.
Treatment Options for PVCs
The treatment for PVCs often depends on the underlying cause and the frequency of occurrences. For patients with benign PVCs, lifestyle modifications may be recommended. This can include reducing caffeine intake, quitting smoking, managing stress, and adopting a heart-healthy diet. It’s akin to tuning a musical instrument to achieve harmony.
In cases where PVCs are symptomatic or frequent, medications may be prescribed. Beta-blockers are commonly used to manage PVCs as they help to regulate heart rhythm. In rare situations, patients may require more invasive treatments such as catheter ablation, which targets the areas of the heart causing the abnormal electrical signals. Understanding EKG Technician Salary: What Can You Expect?
Lifestyle Changes to Manage PVCs
Implementing lifestyle changes can significantly reduce the frequency of PVCs. Consider these strategies:
- Diet: Incorporate fruits, vegetables, whole grains, and lean proteins.
- Exercise: Regular physical activity can strengthen the heart.
- Hydration: Ensure adequate fluid intake, especially if you’re active.
- Stress Management: Techniques like yoga, meditation, or deep breathing can help.
By making these changes, individuals can take proactive steps in managing their heart health.
Prognosis and Long-term Outlook
The long-term outlook for individuals with PVCs varies widely. Many people experience infrequent PVCs that have little to no impact on their overall health. For others, especially those with underlying heart conditions, the presence of PVCs can signal the need for ongoing monitoring and treatment.
Research suggests that while PVCs can be concerning, most individuals with infrequent PVCs do not face significant risks. The key lies in understanding the context of the PVCs and addressing any underlying issues. Regular follow-ups with a healthcare provider can ensure that any changes in heart rhythm are monitored appropriately.
Living with PVCs
Living with PVCs can be daunting, especially if they cause anxiety or discomfort. Education and awareness are empowering. Understanding that many people experience PVCs and that they can be managed is crucial. Regular check-ups, adherence to treatment plans, and making informed lifestyle choices can all contribute to a healthier heart and improved quality of life.
Conclusion
PVCs can present as a perplexing issue for many individuals. However, by understanding what PVCs are, how they manifest on an EKG strip, and their implications for heart health, you can take charge of your cardiovascular wellness. Remember, while PVCs are common, being proactive about your heart health is essential. Always consult your healthcare provider if you notice changes in your heart rhythm or experience concerning symptoms. With the right knowledge and support, you can manage PVCs effectively and maintain a healthy heart.
FAQs
1. What does PVC on an EKG strip look like?
PVCs appear as wide, bizarre QRS complexes that occur earlier than the expected heartbeat, often without a preceding P wave.
2. Are PVCs dangerous?
Most PVCs are benign, but frequent or symptomatic PVCs may require medical evaluation to rule out underlying conditions.
3. How can I reduce PVCs?
Reducing stress, limiting caffeine intake, and maintaining a healthy lifestyle can help decrease the frequency of PVCs.
4. When should I seek medical help for PVCs?
If you experience chest pain, lightheadedness, or increased frequency of PVCs, seek medical attention promptly.
5. Can PVCs lead to other heart problems?
Infrequent PVCs usually don’t lead to serious problems, but frequent PVCs may indicate underlying heart issues that need attention.